Airways
October - December 2016
MTSA Partners with AANA to Offer Acute Surgical Pain Management Fellowship
First cohort to begin in 2017
Middle Tennessee School of Anesthesia is stepping up efforts to better educate nurse anesthetists on surgical pain treatment options that can shorten recovery time and offer more effective ways of managing perioperative care.
MTSA and the American Association of Nurse Anesthetists (AANA) have partnered to offer a postgraduate Acute Surgical Pain Management Fellowship (ASPMF) beginning summer 2017. Both organizations unveiled details at the AANA’s National Congress in Washington, D.C., on Sept. 11.
“We continue to see a growing demand among nurse anesthetists for a better approach to acute surgical pain management,” said Chris Hulin, DNP, MBA, CRNA, President of MTSA. “There are new technologies and advanced intervention techniques that didn’t exist just a few years ago. We felt it was critical to offer a highly specialized program for our students, many of whom have extensive experience and want to stay on the cutting edge of the field. The Acute Surgical Pain Management Fellowship enables them to do that.”
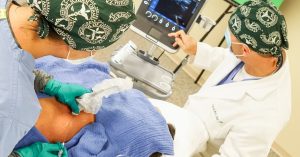 In addition, the Fellowship addresses the growing call to offer anesthesia-based surgical pain treatment options as an alternative to prescription opioids, which continue to be a critical concern among healthcare providers nationwide.
In addition, the Fellowship addresses the growing call to offer anesthesia-based surgical pain treatment options as an alternative to prescription opioids, which continue to be a critical concern among healthcare providers nationwide.
The objective of this new certificate program, a component of the AANA Pain Management Curriculum, is to advance the knowledge and skills of Certified Registered Nurse Anesthetists (CRNAs) in acute surgical pain management and prepare them to help meet the growing need for this evidence-based approach in the United States.
CRNAs = Part of the Solution to a Growing Need
The field of pain management is continually growing. As the baby boom generation ages, increasing numbers of patients will undergo surgery, and CRNAs will be responsible for managing these patients’ acute pain. The Fellowship will equip CRNAs with the necessary knowledge and skill-sets to meet this growing demand. From medical management approaches, such as multimodal therapies and opioid sparing strategies, to advanced interventional techniques, including continuous catheter utilization, CRNAs will acquire the knowledge to treat these patients with confidence and skill.
The Program Process
The ASPMF consists of a classroom component offered via distance education (didactic education) and a clinical component (proctored hands-on clinical experience offered through one or more clinical sites). Fellows will learn innovative techniques including multimodal and interventional therapies to manage acute surgical pain, while developing business management proficiency.
Topics of study include:
• Legal, ethical, and professional issues related to acute surgical pain management
• Psychosocial, spiritual, and cultural dimensions of acute surgical pain
• Non-allopathic considerations for acute surgical pain management
• Physiological aspects of pain
• Assessment and evaluation of the patient with acute surgical pain
• Pharmacogenetics, dynamics, and kinetics related to acute surgical pain management
• Technical interventions for the management of acute pain
• Foundations of initiating an acute pain service
• Business fundamentals in acute pain management
To be admitted, a prospective fellow must be a CRNA with an active, unencumbered license. Completion of a basic and advanced-cadaveric ultrasound-guided regional anesthesia workshop is required prior to enrollment in the program.
About the American Association of Nurse Anesthetists
Founded in 1931 and located in Park Ridge, Ill., the AANA is the professional organization for more than 49,000 nurse anesthetists across the United States. As anesthesia specialists, Certified Registered Nurse Anesthetists (CRNAs) safely provide approximately 40 million anesthetics to patients each year for surgical, obstetrical, pain management, and trauma stabilization services. CRNAs deliver essential healthcare in thousands of communities and are able to prevent gaps in access to anesthesia services, especially in rural, inner-city, and other medically underserved areas of the country. They are highly valued in today’s healthcare environment because they deliver the same safe, high-quality anesthesia care as other anesthesia professionals but at a lower cost, helping to control rising healthcare costs.
Visit mtsa.edu/fellowship for more information.
President’s Message
 Welcome to the newly redesigned Airways! I’m excited to unveil MTSA’s refreshed branding in our quarterly newsletter. We also launched a redesigned website over the summer, all of which reflects our commitment to staying on the cutting-edge of our field while also honoring our rich history and heritage.
Welcome to the newly redesigned Airways! I’m excited to unveil MTSA’s refreshed branding in our quarterly newsletter. We also launched a redesigned website over the summer, all of which reflects our commitment to staying on the cutting-edge of our field while also honoring our rich history and heritage.
As you’ve seen from our cover story in this issue, MTSA is once again expanding into new frontiers of nurse anesthesia with our Acute Surgical Pain Management Fellowship (ASPMF). The new program was spearheaded by Patrick Moss, who has provided invaluable leadership to the School during his tenure.
Unfortunately for MTSA, Patrick has answered the call to return to full-time clinical practice, where he will direct the anesthesia department at a busy outpatient surgery center. With Patrick at the helm, I am confident the center will become a flagship model for a comprehensive outpatient surgical pain management program run by a CRNA. We look forward to partnering with him as his new work location will be a premier regional anesthesia clinical site for the new Fellowship program next summer.
As a way to wish Patrick well and honor his contributions to MTSA, we’re pleased to feature his Capstone in this issue of Airways. In addition, his involvement in the ASPMF has helped us take a leap forward in two unique ways:
1. American Association of Nurse Anesthetists (AANA) Partnership
The AANA had already developed a partnership with Texas Christian University’s Harris College of Nursing & Health Sciences on a Chronic Pain Management Fellowship, which is a post-masters certificate program for CRNAs.
Knowing that MTSA would be the perfect fit to expand into surgical pain management, we joined with the AANA in developing a curriculum for a Fellowship of our own. We saw the need, worked directly, and now we are moving ahead.
The AANA’s national presence will give us added reach to attract Fellowship candidates from across the country. The launch included an announcement at the AANA’s National Congress in Washington, D.C. on Sept. 11, materials distributed to attendees, and multiple placements in their online and print publications.
Our work with the AANA dovetails with our approach that partnerships—such as the ON-Q Center of Excellence with Halyard Health—are vital to MTSA’s continued growth and impact.
2. Solution-based Approach
Not only is the partnership with the AANA a critical element, the ASPMF also addresses a specific skill set that is becoming more in-demand in our field. The opioid crisis in the U.S. has reached epidemic levels. Some of the problems stem from an overreliance on prescription narcotics as the primary method to reduce perioperative pain. However, the use of ultrasound-guided regional anesthesia (USGRA), along with other multimodality interventions, can reduce or eliminate surgical pain without the use of opioids.
The Fellowship answers the need for solutions that rely less on opioids for post-surgical pain, which makes the curriculum something that more CRNAs will need to learn to advance their careers in the changing healthcare environment.
All these elements add up to an innovative program that we’re very proud to offer starting next year. It also shows that we are committed to being the “school of choice” for nurse anesthesia—and both the medical and anesthesia community have taken notice.
Wi-Fi Anesthesia: The Future is Now
A Review of DNAP Graduate Patrick Moss’s Capstone Project

Patrick Moss
DNAP, MS, CRNA, APN
The disparity between rural and urban healthcare is an issue that weighs heavily on Patrick Moss, a 2015 graduate of MTSA’s DNAP program. It is especially prevalent in nurse anesthesia, which is why Moss decided to take a deep dive into remote education with his Capstone project: Telementoring During the Performance of Ultrasound-Guided Regional Anesthesia (USGRA): Perspectives of Student Registered Nurse Anesthetists.
The purpose of his Capstone project was to examine the feasibility of the telementoring process during the performance of USGRA by student registered nurse anesthetists (SRNAs).
“Providing remote nurse anesthesia training and education in underserved areas is vitally important,” Moss said, adding that enormous differences exist between high and low socioeconomic environments. “There are also huge legal and compliance hurdles to jump to make telemedicine a reality in our field, but through this project I found that it can be accomplished under the right conditions.”
Moss’s Capstone revealed that:
• There exists a supply and demand issue for the service of USGRA. Few practicing certified registered nurse anesthetists (CRNAs) have been formally educated in the skills necessary to perform regional anesthesia utilizing ultrasound guidance, a technology used to enhance patient satisfaction and improve the overall success rate.
• Practicing CRNAs have options to increase knowledge and skill in USGRA through online, or in-person, courses; however, according to the American Association of Nurse Anesthetist’s (AANA) department of continuing education, none of the USGRA programs offer post-course mentoring.
• The use of telementoring, (i.e., mentoring from a distance) could be used to support and increase CRNA’s confidence and skill development after the foundational learning experience.
“To conduct the project, I recruited students to serve as facilitators who were to perform techniques they had never been taught before. I logged in via remote video and audio connection from a different location and guided them through the process. The results were very encouraging, as I discovered that each student was able to perform the intervention successfully. This interaction between student and instructor was aided by Wi-Fi technology,” Moss said.
Immediately following each telementoring session, participants completed a short survey that contained both quantitative and qualitative questions, which provided additional feedback for analysis.
“There are still a lot of open questions we need to address to standardize telementoring in anesthesia and make it more readily available across the country,” Moss added. “For example: What are liabilities for the remote clinician? Does the remote clinic need to be credentialed in the facility or state where it’s taking place? How does the reimbursement work? Some of these questions have been addressed in other fields, but not for USGRA.”
According to Moss, the project’s findings were consistent with that of other telementoring feasibility studies within the field of surgical medicine. Although no telementoring studies exist from the specialty of nurse anesthesia, parallels can be drawn from this project’s findings, including strengths such as local clinician’s confidence, efficiency, guidance, work, success, and ultimately, patient safety as well as potential limitations including informational technology, network, legal, and licensure practices.
Moss concluded that USGRA telementoring of anesthesia providers is feasible, likely to provide anesthetists with increased confidence, and result in improved patient safety. Based on the findings, and those previously published, he found it reasonable to assume that telementoring may improve anesthesia-related outcomes and quality of life, especially when compared to traditional, opioid-based, acute pain management techniques.
“It’s a tragedy that in our country not all patients have equal access to healthcare, especially in anesthesia. But I’m encouraged that we can change this through telementoring, and I hope more research can be performed to make that a reality,” Moss said.
Following are excerpts from a broader discussion with Moss related to his Capstone project.
Airways: What led you to tackle this particular issue?
Patrick Moss: I wanted to focus on ultrasound-guided regional anesthesia. I leaned heavily on my committee chairs, Dr. Maria Overstreet, and Dr. Michael Vollman. Through their mentorship, I realized that feasibility was not only possible but applicable. There are no papers published in telementoring in nurse anesthesia. I had to use literature from other disciplines.
Airways: How much of telementoring relies on the human element, having a good teacher?
P.M.: As a teacher, to be on the same wavelength as the clinician is critical. What makes it challenging are the legal and compliance hurdles that make it possible to have two sets of clinicians working in locations, often in different states, that have different standards and requirements.
Airways: What was the most difficult part of completing the project?
P.M.: It was difficult early on to narrow the focus to something I could accomplish within one year. What I found was that your committee will continuously refocus you and continue to encourage you.
Airways: What was the most rewarding part of the project?
P.M.: I really enjoyed being able to share my research with the students and empower them to continue seeking knowledge, no matter how many degrees they might have.
Airways: What are some outcomes you hope to see from this project?
P.M.: I hope through this project, others will find an interest in telementoring in anesthesia and promote further research. We’re constantly looking for ways to achieve more effective avenues of training and educating CRNAs. I think this is a strong contender. Now we just need others to take it further.
After eight years of service at MTSA, Patrick Moss is leaving his full-time role to become director of the anesthesia department at an outpatient surgery center. His work at the School has helped countless students reach the highest levels in the field of nurse anesthesia. And he has been instrumental in launching the Acute Surgical Pain Management Fellowship, which will begin next summer.
Patrick will continue his involvement with the Halyard Health Center of Excellence by training CRNAs in both the Basic and Advanced Regional Anesthesia Workshops on MTSA’s campus.
“I hope you’ll join me in showing your appreciation for Patrick’s hard work and dedication,” said Chris Hulin, MTSA’s president. “We wish him great success in his new role. He will certainly be missed.”
Participants Gear Up for Haiti Mission
Group requests donations, prayers for successful trip

MTSA’s mission team is anticipating a successful trip to Haiti Oct. 23-30, which will include providing Acute Surgical Pain Management (ASPM) care for a surgical hand team at Hopital Adventiste d’Haiti, and holding continuing education sessions and placing ultrasound machines into service at both the Visitation Clinic in the Nippes region and at Hopital Adventiste d’Haiti in Carrefour.
The mission is focused on providing a lasting effect by giving local practitioners the tools and education they need for ongoing care of their patients, including a day-long nursing workshop on basic patient assessment and evaluation.
As part of the efforts, Tenvision has donated an ultrasound machine that will be used by midwives and physicians of Visitation Clinic. In addition, Halyard Health has generously donated block procedure trays for the hand surgeries.
Participants in the mission have requested anyone interested in donating can still do so by visiting www.mtsa.edu/donate. Prayers of support are also appreciated.
For additional information about the mission trip, visit www.mtsa.edu/haiti-mission.
Project Stethoscope
The Haiti Mission team is asking for help from alumni, students and friends of the School to donate stethoscopes for the trip!
It’s an unfortunate reality in Haiti that there aren’t enough stethoscopes to enable all nurses to have one. In fact, there’s typically only one scope per unit. Your donated scope will go to a nurse at the Hopital Adventiste d’Haiti, where MTSA administration, faculty, and students are headed Oct. 23-30.
Please bring your donations to MTSA’s Administrative office in the Magan Building or ship to 312 Hospital Drive, Madison, TN 37115, before Oct. 19.
MTSA Welcomes New Assistant Program Administrators
“As MTSA continues to meet increasing demands for the Acute Surgical Pain Management Fellowship, and as we transition into the DNAP entry-to-practice program, I am pleased to announce the following assistant program administrator appointments,” said Chris Hulin, DNP, MBA, CRNA.
 William “Bill” Johnson, DNAP, CRNA
William “Bill” Johnson, DNAP, CRNA
Director, Center of Excellence for Acute Pain Management
Assistant Program Administrator
Bill will be joining the MTSA family in November and will begin teaching immediately. He will focus on the regional anesthesia classes and the new Acute Surgical Pain Management Fellowship. He was a faculty member at Texas Wesleyan University and Texas Christian University and currently practices at John Peter Smith Hospital in Fort Worth, Texas.
 Russell “Rusty” Gentry, DNAP, MSNA, MSN, CRNA
Russell “Rusty” Gentry, DNAP, MSNA, MSN, CRNA
Assistant Program Administrator
Rusty will join MTSA at the end of the year and will begin his duties in 2017. He will give guidance to our accreditation requirements and will teach a broad base of classes. He is currently the Associate Program Administrator of the Florida State University Nurse Anesthesia Program in Panama City and has served as an interim director. In addition to being a nurse practitioner, his anesthesia experience includes cardiac/thoracic, and he currently practices at an outpatient surgery clinic.
Golfing for Haiti
13th annual MTSA Golf Classic benefits Mission Initiative
A beautiful late summer day greeted golfers at the 13th Annual MTSA Golf Classic held on Sept. 15. The field of 100 participants enjoyed the outing, which resulted in a net contribution to MTSA of more than $21,500.
“The event proceeds will help fund MTSA’s Mission Initiative in Haiti and the surrounding communities,” said Jim Closser, Vice President for Advancement & Alumni.
The event was held at Hermitage Golf Course – General’s Retreat and began with lunch and concluded with a full dinner. “It’s the generosity of the major sponsors which contributes so much to the success of this golf outing,” Closser said. “We are grateful for each player and sponsor that makes this day so successful.”
Major sponsors:
• Dinner: Cardiovascular Anesthesiologists, PC
• Drink/Snack Carts: PBG Builders, Inc.
• Holes-in-One: Harold Green, Mass Mutual Insurance
• Longest Drive: Anesthesia Medical Group, LLC
• Skill Prize Sponsor: The Mollenkopf Design Group, LLC
• Team Photo: M3 Technology Group
Next year’s tournament will be held on Sept. 21, 2017, at Hermitage Golf Course.
Class of 2018 Recognized at White Coat Ceremony

The annual White Coat Ceremony was held on Thursday, Aug. 25, at the Madison Campus Seventh-day Adventist Church.
MTSA Alumni Ballot Mailed
The ballot to elect 2017 MTSA Alumni Officers and Decade Representatives was mailed earlier this month to all MTSA alumni, said Alumni President Max Fort (’97) CRNA, MS, APN. “Please take a few minutes to complete your ballot and return it to the MTSA Alumni Office before the October 27 deadline.”
In accordance with MTSA Alumni Association Bylaws, this ballot must be returned and in-hand at the MTSA Alumni Office by close-of-business on Thursday, Oct. 27, to be counted. The ballot received includes the following nominees:
> President: Mathew O’Connor (’07)
> Secretary: Lisa Michelle Clark Humphrey (’03)
> 2010’s Rep: Matt Fosnot (’10)
> 1990’s Rep: Kevin Burns (’99)
> 1980’s Rep: Roxanne Lentz (’82)
> Rep-at-Large: Trevor Eldred (’03)
All MTSA Alumni are invited to attend the MTSA Alumni Association Annual Business meeting to confirm the ballot results. This meeting will be held at MTSA on Tuesday, Nov. 1, at 4:30 p.m. Central Daylight Time. Votes must be cast on the official ballot to be considered valid. If you have any questions, please call (615) 732-7674, or e-mail jclosser@mtsa.edu.
Class of 2016 Graduation Ceremony
MTSA graduation exercises are scheduled for Friday, Nov. 18, at the Madison Campus Seventh-day Adventist Church. The ceremony will begin at 10 a.m. and will be followed by an open house on the School’s campus located adjacent to the church. Refreshments will be served.
History in the Making

Members from the MTSA Class of 1973 share lunch in the Madison Hospital cafeteria. (l to r) Julie Fernandez, Instructor Bettie Matthews (’71), Sylvia Evans, Carole Kaufman, Bill Gerrez, and Jane Frost. This photo was submitted by Carole Kaufman who said, “I graduated in 1973 from the Madison Hospital School of Anesthesia and am now retired. I loved my job where I worked in the operating room of Baptist Hospital for 37 years. I want to share this photo showing fun times and reminding us of the good-ole-days with Mr. Bowen, Mrs. Ackerman, Mrs. DeVasher, and others who helped us become CRNAs. Thank you MTSA!”








