MTSA Welcomes Richie Flowers as Program Administrator
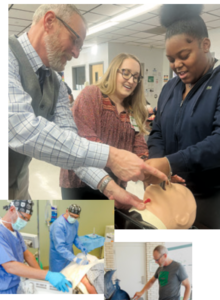
Middle Tennessee School of Anesthesia (MTSA) has announced the appointment of Richard “Richie” W. Flowers Jr. (pictured, right), DNP, CRNA, CHSE, FAANA, as Program Administrator.
Beginning in January 2025, Flowers will lead MTSA’s flagship program, the Doctor of Nurse Anesthesia Practice (DNAP), bringing a broad range of experience in both the academic and clinical settings. He is also an MTSA alumnus, earning a Master of Science with a focus in Nurse Anesthesia degree in 1997.
“I’m excited to go back to where my journey to becoming a CRNA began 30 years ago next year!” Flowers said. “Having the opportunity to lead such a prestigious program is truly an honor and privilege. It feels like this is where I belong, and I can’t wait to be home.”
Flowers currently is Assistant Professor, Department of Academic Nursing, Wake Forest University School of Medicine, where he has served in various academic and leadership roles since 2015. Prior to that, he worked as a CRNA in numerous clinical practice environments, including owning his own practice.
“We are thrilled to welcome Dr. Flowers ‘back’ to MTSA!” said President Chris Hulin, DNP, MBA, CRNA. “His background in the clinical setting, combined with his experience at Wake Forest as well as serving on non-profit boards and professional organizations, has uniquely positioned him to excel in program administration. We have the utmost confidence in his ability to take MTSA’s program to the next level.”
“I firmly believe that you have to know where you’ve been to fully understand where you are going,” Flowers added. “I’m eager to engage with the staff, faculty, learners, alumni, and stakeholders of MTSA to learn about what makes it such a special place so that our vision for the future embraces the incredible legacy of the past. MTSA has a long history of producing excellent CRNAs, and I look forward to not only continuing this legacy but making sure we are preparing our graduates for the exciting opportunities they will have in the future.”
Flowers earned his Doctor of Nurse Practice (DNP) degree from Baylor College of Medicine, a Master of Science from MTSA, and a Bachelor of Science in Nursing (BSN) from Memphis State University.
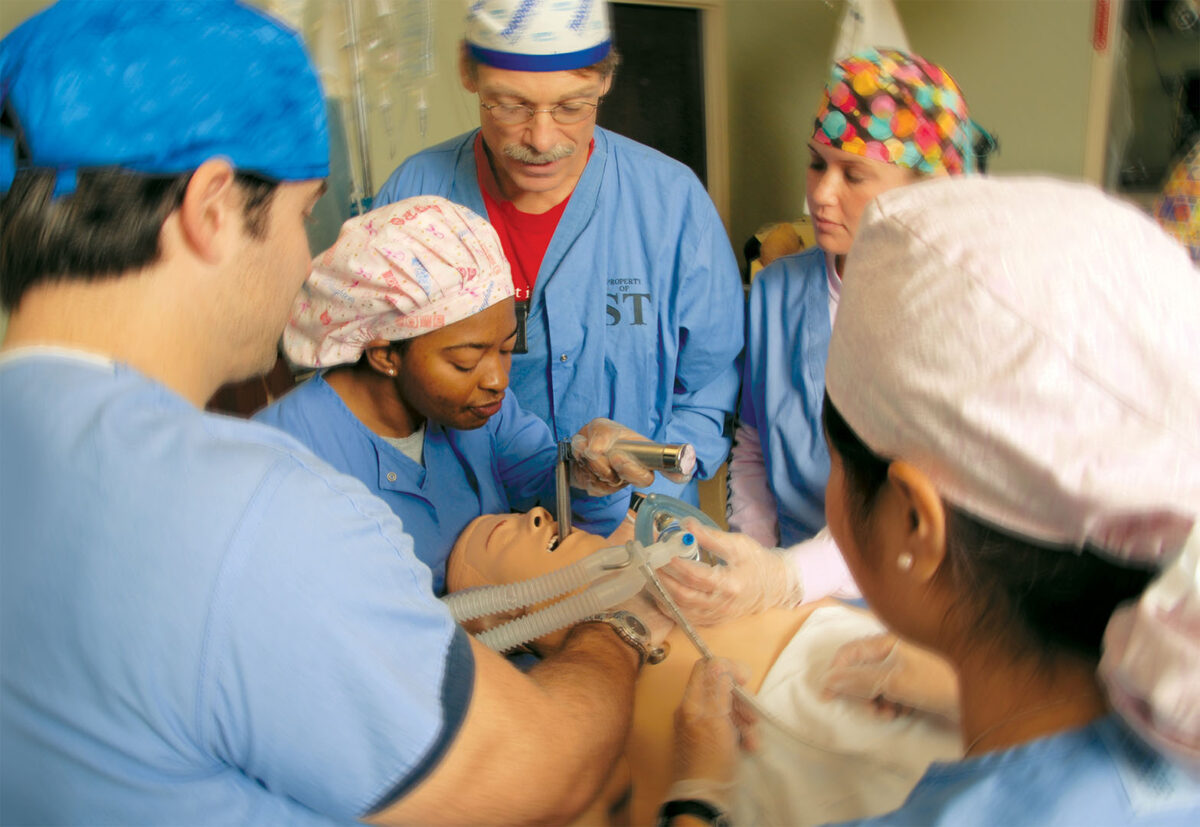
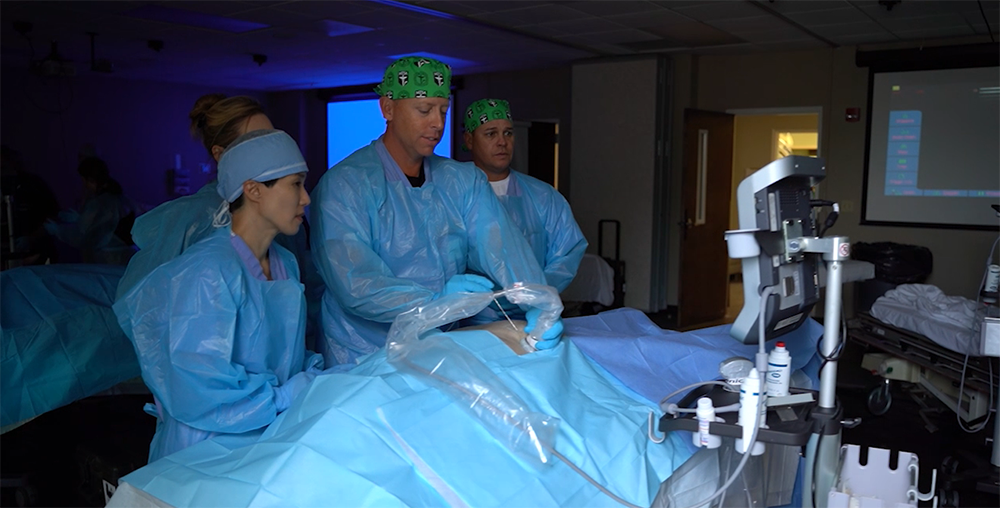
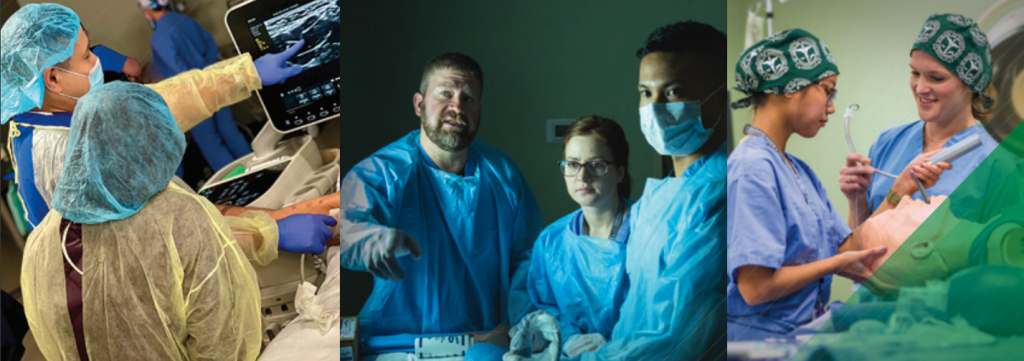
MTSA’s Practice Doctorate/DNAP program is a full-time course of study for 36 consecutive months, on the campus of MTSA. It prepares learners to become experts in providing anesthesia care in a wide range of settings, applying evidence-based practices and improving patient outcomes. The program features a rigorous clinical rotation process that offers students a vast array of clinical experiences in the peri-anesthesia setting.
About Middle Tennessee School of Anesthesia
Founded in 1950, Middle Tennessee School of Anesthesia (MTSA) provides graduate-level education and training of nurse anesthetists in a Christian environment born of its Seventh-day Adventist heritage. MTSA is the only independent, fully accredited anesthesia institution of its kind in the nation, instilling excellence through innovative and diverse clinical experience. More than 75% of Middle Tennesseans having surgery entrust their lives to its graduates on a daily basis. A leader in academic, clinical and professional distinction, MTSA is responsive to the needs of its constituents, providing affordable graduate education for students from diverse backgrounds. For more information, visit www.mtsa.edu.