Airways
February 2023
Using Opioid Free Anesthesia with Robotic-Assisted Prostatectomy
This issue features a synopsis of research by the husband-and-wife team of Keven Keller, CRNA, and Katie Keller, CRNA, both MTSA graduates (pictured above). Their research was submitted for publishing in the Journal of PeriAnesthesia Nursing and continues the trend of MTSA graduates helping to advance opioid-sparing interventions and promoting evidence-based practice.
“The experience Katie and I had at MTSA put us head-and-shoulders above others we worked with because the clinical situations truly prepared us to be independent CRNAs.” – Keven Keller, CRNA, Class of 2013
TITLE: Short-Term Patient Outcomes after Implementation of Robotic-Assisted Radical Prostatectomy under Opioid Free Anesthesia at an Ambulatory Surgery Center
AUTHORS: Keven Keller, Katherine Keller, Thomas Baribeault, and Kenneth A. Wofford
SYNOPSIS: Opioid free anesthesia (OFA) is associated with decreased risk of postoperative nausea and vomiting (PONV) and need for rescue analgesia, making it ideal for patients anticipating same-day discharge. The purpose of this project was to describe the perioperative care and short-term outcomes for patients undergoing robotic-assisted radical prostatectomy (RARP) under OFA at an ambulatory surgical center (ASC).
A retrospective descriptive design was utilized to examine the perioperative care and short-term outcomes of patients undergoing RARP under OFA at an ASC.
The records of all sequential patients undergoing RARP over an 18-month period were reviewed. Data collected included patient comorbidities, surgical procedures, pre-, intra-, and post- medications administered, verbal numeric rating scale (VNRS) for pain scores, times to oral intake, ambulation, and discharge, patient disposition, and unplanned return to the ER or hospital within 30 days.
Data were extracted from 54 sequential records. Median VNRS scores were zero throughout PACU stay. Fifty-three patients (98.1%) were successfully discharged home, with an average postoperative stay of 250.8 (SD 35.0) minutes. There were no complaints of post-discharge nausea and vomiting or intractable pain at 72 hours after surgery. One patient was transferred to hospital and two patients returned to the emergency room within 30 days.
Conclusions: Although generalizability is limited, these results suggest that carefully selected patients can be discharged home after RARP under a balanced OFA technique. Innovative practices are needed to address the current backlog of patients needing non-emergent surgery. Discharge home avoids the increase in resource consumption and infection risk associated with hospital admission.
About the Authors
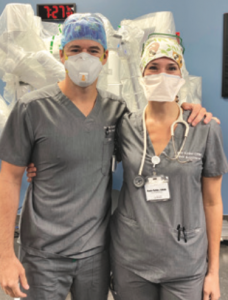 Keven and Katie Keller are the founders and co-CEOs of Keller Anesthesia LLC in Atlanta. Formed in 2016, their group provides services at nine surgery centers in metro Atlanta, all focused on urology and gynecology. With 24 CRNAs on staff, their most common cases include kidney stone treatments, prostate biopsies, bladder tumors, vaginal repairs and hysterectomies.
Keven and Katie Keller are the founders and co-CEOs of Keller Anesthesia LLC in Atlanta. Formed in 2016, their group provides services at nine surgery centers in metro Atlanta, all focused on urology and gynecology. With 24 CRNAs on staff, their most common cases include kidney stone treatments, prostate biopsies, bladder tumors, vaginal repairs and hysterectomies.
Keven and Katie met while working as ICU nurses at Atlanta Medical Center. Both applied and were accepted to MTSA at same time, graduating from the Master’s program in 2013 and getting married the same year. They now have two daughters, Brinley, age 5, and Adeline, age 4.
“We managed to make it through anesthesia school together, so we figured this marriage is going to be rock solid,” Keven said. “When it comes to balancing our personal and professional life together, we like to say, ‘teamwork makes the dream work.’”
“We’ve always done everything together. It’s a partnership,” Katie said. “We bounce ideas off each other, and we both have areas of strength that are different but complementary.”
The Kellers’ research began as an attempt to minimize or eliminate opioid usage and enable quicker recovery by surgical patients. They were initially hesitant but, after extensive training, they were able to design an opioid-free ERAS urology protocol. It includes not only pre-op protocols but also steps to take several days prior to help prep patients all the way through the post-op period.
“From our research, we’re the first group to be able to do robotic prostatectomy at an ambulatory surgery center without opioids. For these and other applicable cases, this is a great option because it costs less. Being able to offer this to patients safely and to have better outcomes is a game changer,” Keven said.
 One aspect of their research that they found most surprising was the negative sequela associated with opioid use. They recognized the pain reflex was much higher when opioids are used versus none at all. And there are many other negative side effects, such as longer lengths of stay, altered mental status, ileus and respiratory depression.
One aspect of their research that they found most surprising was the negative sequela associated with opioid use. They recognized the pain reflex was much higher when opioids are used versus none at all. And there are many other negative side effects, such as longer lengths of stay, altered mental status, ileus and respiratory depression.
“It was shocking to realize how we’ve always practiced surgical pain management, when better alternatives are often available. It’s amazing that we can get patients in and out of a surgery center the same day. And the patients are blown away. They come in expecting to hurt and instead then they’re able to get up and leave within a matter of hours,” Katie said.
The Kellers both mentioned their experience at MTSA as a critical element of their success as CRNAs.
“MTSA’s program in general – the fact that we went to so many different clinical sites – gave us a variety of learning environments. I don’t know that we could have accomplished so much early on in our careers without that,” Katie said.
“We’re really grateful to MTSA and President Chris Hulin for giving us the opportunity. The school has done a phenomenal job. The experience Katie and I had at MTSA put us head-and-shoulders above others we worked with because the clinical situations truly prepared us to be independent CRNAs. Also, [MTSA Dean Emerita] Ikey DeVasher was there at the time. She and her husband, Bernard, were strong, faith-based leaders who really set us up for success,” Keven added.
President’s Message: Propelling Our Strategic Plans

Chris Hulin, DNP, MBA, CRNA
President
I’m pleased to announce two important changes to our leadership team that will continue to strengthen MTSA’s strategic plans. First is the addition of Christian Falyar, DNAP, CRNA, FAANA, as Director of the Acute Surgical Pain Management (ASPM) Fellowship at Middle Tennessee School of Anesthesia.
As a former board-certified sonographer, Dr. Falyar has been involved in ultrasound training and education for over 20 years. He has a diverse anesthesia background, working both in independent private practice and serving on faculty at several schools of nurse anesthesia. He most recently served as the Assistant Director of the Nurse Anesthesia Program at Duke University, in Durham, NC. Read more about Dr. Falyar and the changes coming to the ASPM Fellowship and continuing education in this issue.
In addition, Hallie Evans, DNP, CRNA, has been promoted to Director of the Doctor of Nurse Anesthesia Practice Completion Program. Dr. Evans began educating in 2009 as a clinical educator and preceptor for nurse anesthesiology students as well as a mentor for scholarly projects. In 2015, she returned to MTSA after serving as faculty at Florida International University while maintaining a strong clinical practice throughout her academic career.
Dr. Falyar and Dr. Evans are taking the baton from Dr. Bill Johnson, who skillfully led the ASPM Fellowship as well as MTSA’s Doctorate Completion program. I would like to add my gratitude for Dr. Johnson’s service these past several years. Because of his dedication, these programs have grown exponentially, and he has developed partner relationships that have been instrumental in our Fellows’ success. I wish him all the best on his next endeavor.
This transition represents a continuation of MTSA’s strategic plans to deliver an exceptional student experience that attracts premier applicants, promotes individual achievement, and results in a clinically excellent practitioner. In addition, we are committed to advancing CRNA practice in ultrasound and pain management through education, strategic partnerships, and distinguished scholarship. Thanks to all our amazing faculty and staff for carrying forward this vision!
Service in Action

A group from MTSA, including staff and a current student, volunteered to pack medical supplies for Project Cure. The organization’s mission includes delivering medical supplies and equipment to developing countries.

MTSA staff volunteered at The Bridge, Inc. to help pack snack bags for the Bridge to Kids, which supports nearly 4,000 students across the Metro Nashville Public Schools system.

MTSA staff volunteered at Exceptional Minds Learning Academy to help organize their storage building and repurpose rooms for a computer lab and kitchen. In addition, staff and students worked on a landscaping project.

Nearly 100 Class of 2024 students, along with faculty and staff, participated in the recent Rise Against Hunger service event on campus. The group packed an astonishing 25,000 meals in just under 90 minutes! The meals will be shipped to people in need around the globe.
Changes Coming to the Acute Surgical Pain Management Fellowship

The growth and evolution of MTSA’s cutting-edge Acute Surgical Pain Management Fellowship (ASPMF) continues as it welcomes a new Director, Christian Falyar, DNAP, CRNA, FAANA.
 Dr. Falyar comes to MTSA from Duke University, where he served as the Assistant Director of the Nurse Anesthesia Program, ranked #3 in the country. He is also joined by the new Assistant Director of the Fellowship, Nicolette Hooge, DNP, CRNA, MBA. Dr. Hooge also comes from Duke University where she worked at the Ambulatory Surgery Center and served as Adjunct Faculty in the Nurse Anesthesia Program.
Dr. Falyar comes to MTSA from Duke University, where he served as the Assistant Director of the Nurse Anesthesia Program, ranked #3 in the country. He is also joined by the new Assistant Director of the Fellowship, Nicolette Hooge, DNP, CRNA, MBA. Dr. Hooge also comes from Duke University where she worked at the Ambulatory Surgery Center and served as Adjunct Faculty in the Nurse Anesthesia Program.
Building on the Fellowship’s early success, Falyar will be working to add content experts and develop relationships with clinical sites to further enhance fellow training.
“Our focus will be an early emphasis on technical skills. We will introduce ultrasound scanning and sonoanatomy related to regional procedures from the beginning, as it is the foundation of everything we do,” Falyar said.
The Fellowship is divided into three semesters over 12 months. Each semester includes a didactic and concomitant clinical course that builds upon the previous one. Program highlights include:
- An international, multidisciplinary faculty
- Instruction in over 50 regional anesthesia techniques
- Clinical sites nationwide offering a wide range of experiences
- Development and incorporation of ERAS protocols into practice
- Essential Point-of-Care Ultrasound (POCUS) training
- Specialty clinical rotation in transitional pain management option
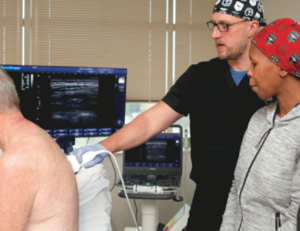 An on-campus intensive during the first week of the Fellowship allows faculty to evaluate the students’ regional anesthesia skills, assessing strengths as well as opportunities for growth. This allows clinical rotations to be tailored towards each individual’s skill set. Fellows who are more advanced will be able to enter clinical practice earlier in the program.
An on-campus intensive during the first week of the Fellowship allows faculty to evaluate the students’ regional anesthesia skills, assessing strengths as well as opportunities for growth. This allows clinical rotations to be tailored towards each individual’s skill set. Fellows who are more advanced will be able to enter clinical practice earlier in the program.
In addition to learning regional anesthesia techniques, a major part of the curriculum is dedicated to understanding pain. Students learn how pain is generated, recognizing it’s not just through one receptor or mechanism. Once they understand these concepts and the different modalities available to address pain, the options for treatment become more numerous, and most are opioid-sparing.
An enhancement planned for the Fellowship is a module on transitional pain medicine, which addresses chronic pain syndromes. The training will center on ultrasound-guided procedures, which differs from the tradition use of fluoroscopy guidance. This will give providers another tool to treat chronic pain without relying on pharmacologic interventions.
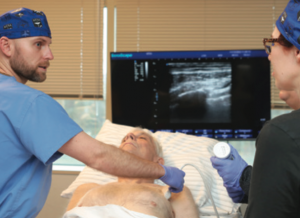 Falyar regards these and other types of procedures as central to the Fellowship’s offering, building knowledge and confidence so providers have a wider range of interventions beyond the basic regional procedures.
Falyar regards these and other types of procedures as central to the Fellowship’s offering, building knowledge and confidence so providers have a wider range of interventions beyond the basic regional procedures.
“At the end of the day, the Fellowship is about developing providers who are skilled in patient care, no matter where they practice or in what environment. The number one goal is to perform safe, efficacious procedures that improve patient outcomes,” Falyar added.
For 2023, MTSA is offering a single cohort in the fall. The application deadline is May 1. For more information, visit mtsa.edu/fellowship.
Student Standouts

Jeff Ferguson (Class of 2022) presented his Doctoral Scholarly work titled, Quadratus Lumborum Block and Transversus Abdominis Plane Block in Non-emergency Cesarean Delivery: A Systematic Review and Meta-Analysis, at the Ohio State University Advanced Practice Provider Conference. His daughter (pictured) attended to watch and support him. (Project Team: Tito D. Tubog, Hallie Evans, Bill Johnson, Jamie Furstein)
Dr. John Edwards and Dr. Stace Dollar (Class of 2021) continue to disseminate their scholarly works on Education and Disposal Methods of Unused Opioids. They were recently interviewed by DisposeRx on their scholarly works.

Caitlin Douglas and William Fuller presented at the VA hospital about the effectiveness of Decadron versus Dexmeditomidine within peripheral nerve blocks. They presented to the anesthesia department, which consisted of anesthesiologists and CRNAs. Afterward one of the anesthesiologists informed them that he had been considering adding Decadron to nerve blocks and their presentation solidified his decision to do so later that day for a patient.

Rose Vernot presented Barriers and Solutions to Accreditation of Anesthesia Program in Low Income Countries on behalf of the Sigma Theta Tau Conference in Denver.
Phyllis Stowe (Class of 2022) presented her Doctoral Scholarly project, Perioperative Anesthesia Handoff Practices and Effects on Effective Communication Exchanges: A Systematic Review and Best Practice Tool, at the Academy of Medical Surgical Nurses Conference in San Antonio, Texas. (Project Team: Hallie Evans, Christian Falyar, Bill Johnson, Janet Forren)
Several MTSA students have presented at different conferences, covering a variety of topics, including the AANA Congress in Chicago.

MTSA students Erasmo Coutino and Mandeep Kaur. Coutino presented “Cadaver-Based Simulation in Ultrasound-Guided Regional Anesthesia: Luxury or Necessity? A Systematic Review.” Kaur presented “Perceptions of Regional Anesthesia Competency In Newly Graduated Nurse Anesthetists: A Cross-Sectional Survey.”

MTSA students Mandeep Kaur and Jamilia Adams-Henderson. Adams-Henderson presented “Acute Pain Management Using Pharmacogenetic Markers to Optimize Perioperative Acute Pain Treatment: A Current Review.”
19th Annual MTSA Golf Classic

Players enjoyed an un-fore-gettable day at the 19th Annual MTSA Golf Classic. The tournament featured multiple flights of four-person teams, culminating in a championship playoff on the 18th hole.
The event supported MTSA’s Mission Initiative in Guyana, where the school provides equipment and simulation training for nursing students studying to be CRNAs. Funding for medical supplies and education curricula for this program makes a lasting impact by improving patient care in this under-developed country.
Tournament Awardees
Overall Champion Winners (pictured above): Chad Anderson, James Cobb, Patrick Jackson and Mark Montgomery
Closest to the Pin:
Hole 3: Joni Kies
Hole 5: Rusty Gentry
Hole 13: Miriam Kleine-Kracht
Hole 17: Matt Ridings
Long Drive: Kirk Larson


About the Guyana Mission Initiative
MTSA doctoral student Lani Hensel, CRNA with Michigan-based Anesthesia Associates of Battle Creek, uncovered specific educational needs in the Guyana program that MTSA is helping to address.
Hensel’s research comprised a literature review on nurse anesthesia simulation in low-resource areas such as Guyana. She incorporated a simulation educational needs survey of nurse anesthetists, which revealed knowledge gaps and highlighted scenarios in which supplemental training and equipment would be beneficial.
“One of the most important skills in anesthesia is crisis-emergency care, and the best way to review and practice those situations is simulation because it’s the safest way,” Hensel said. “Our goal is to raise funds to be able to take more advanced simulation equipment to the program in Guyana and help the anesthetists and students with scenarios where their confidence level can be improved.”
Now Open: Enrollment for 2023 Nurse Anesthesia Programs
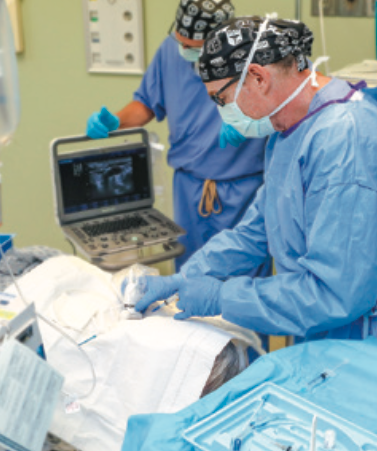
MTSA is now accepting applications for a wide range of nurse anesthesia programs to help you excel as a CRNA. Visit mtsa.edu/apply for details.
Doctor of Nurse Anesthesia Practice (DNAP)
 For RNs: DNAP Entry to Practice Program
For RNs: DNAP Entry to Practice Program
Deadline to apply: May 31
MTSA offers the DNAP Practice Doctorate to registered nurses who have met each of the application requirements for admission. The DNAP Practice Doctorate is a full-time course of study for 36 consecutive months. For more information, visit mtsa.edu/practicedoctorate.
For CRNAs: DNAP Completion Program
Deadline to apply: May 1
The DNAP Completion program is specifically designed with the working CRNA in mind and in an online format. All students accepted into the program must be currently licensed CRNAs. The program can be completed over two years. For more information, visit mtsa.edu/doctorate.
 Nurse Educator Certificate Program
Nurse Educator Certificate Program
Deadline to apply: May 1
MTSA’s Nurse Educator Certificate Program is a 12-month course of study that prepares students to function in the Nurse Educator role. Students learn about the theoretical foundations of nursing education, how to assess educational needs, various evidence-based teaching and assessment strategies, curriculum design and development, and program evaluation. For more information, visit mtsa.edu/nurseeducator.
Nurse Faculty Loan Program
Admitted students in the Nurse Educator Certificate Program may be eligible for HRSA Nurse Faculty Loan program (NFLP) with a 4-year nurse educator employment commitment post-graduation which provides 85% loan forgiveness when this educator employment is completed. For more information, visit mtsa.edu/nflp.
Acute Surgical Pain Management Fellowship
As the only fellowship of its kind for CRNAs in the United States, the Acute Surgical Pain Management Fellowship (ASPMF) meets the growing need for an evidence-based approach to optimize patient care throughout the perioperative continuum. The goal of this post-graduate certificate program, part of the AANA Pain Management Curriculum, is to provide CRNAs a path to expand their current regional anesthesia skillset in the treatment of acute postsurgical pain.
The Fellowship is a hybrid program, using a combination of on-campus intensives, online (didactic) education, cadaveric workshops, and clinical experiences with experienced preceptors to teach providers the necessary skills to manage acute surgical pain and improve patient outcomes throughout the perioperative period.
For 2023, MTSA is offering a single cohort in the fall. ASPMF application cycle and deadlines are as follows:
Application deadline – May 1, 2023
Interviews begin – June 1, 2023
Semester starts – Sept. 5, 2023
MTSA offers dual enrollment in the Doctor of Nurse Anesthesia Practice (DNAP) Completion program along with the Fellowship or the Nurse Educator Certificate Program, allowing students to complete two academic tracks at once!
For more information, email Terry Owens at terry.owens@mtsa.edu, or visit mtsa.edu/fellowship.
 Regional Cadaveric Workshops
Regional Cadaveric Workshops
Ultrasound-guided regional anesthesia cadaveric workshops at MTSA incorporate anatomic dissection, live model scanning, and procedural cadavers to provide a comprehensive overview of the regional anesthesia procedures commonly used in the management of perioperative pain. The workshops are clinically focused, and techniques learned are easily translated into a provider’s daily practice.
Prior to the workshop, participants complete online modules detailing the important aspects of the blocks to be covered. This allows attendees to focus on improving scanning and needling techniques during the workshop. A low student-to-faculty ratio (approximately 4:1) ensures participants receive individualized attention and maximum scanning times (up to six hours).
2023 Workshop Schedule:
March 26 – Basic Regional Cadaveric Workshop [SOLD OUT]
Sept. 10 – Basic Regional Cadaveric Workshop
May 7 – Advanced Regional Cadaveric Workshop
Oct. 1 – Advanced Regional Cadaveric Workshop
For more information, email Terry Owens at terry.owens@mtsa.edu, or visit mtsa.edu/workshops.
9th Annual MTSA Mission & Awards Gala
Presenting Sponsor: U.S. Anesthesia Partners – Anesthesia Medical Group
MTSA invites you to join colleagues and friends for an evening of celebration, dining and silent auction at the 9th Annual Mission & Awards Gala benefiting MTSA’s Mission Initiatives both locally and abroad. Each year, proceeds from the event fund supplies, education curricula, and other needed items for mission activities.
This year’s Gala will focus on specific needs for women and children of Iquitos, Peru. The School is partnering with the People of Peru Project in planning an international service opportunity that will allow all MTSA staff to participate. The partnership will also help support anesthesia care in a future clinic with two operating rooms focusing on surgery for those in extreme poverty.
To purchase individual tickets, sponsorships or tables, visit mtsa.edu/gala. For more information, email marketing@mtsa.edu.
Date: Saturday, March 4, 2023
Location: The Hutton Hotel, Vista Ballroom
Reception/Silent Auction: 6 p.m.
Dinner: 7 p.m.
 A Message from Gala Committee Co-Chair Deana Vandivier, CRNA
A Message from Gala Committee Co-Chair Deana Vandivier, CRNA
I am so excited to be the 2023 MTSA Gala committee co-chair. My wish for this year’s Gala is to convey the difference each of us makes by supporting this wonderful and annual event. Whether your support is by attending the Gala or in the form of a donation, collectively each of us can make a difference when working towards a common goal.
The Gala is the perfect occasion to reconnect with friends and colleagues, and in an effort to make it easier for more of our friends and colleagues to attend, relax and enjoy this event, the date of this year’s Gala is on Saturday, March 4. Although the day of the week for the Gala has changed to a Saturday evening, so many of your favorite things about the Gala have not changed, such as having a delicious meal at a fabulous venue, the chance to get dressed up, bid on silent auction items, listen to live music from our own talented music city healthcare professionals, and of course celebrate the amazing leadership and work of our much deserving anesthesia friends and colleagues.
I hope to see each of you on March 4 as we commemorate another MTSA Gala!
About the Awards
MTSA’s Mission & Awards Gala includes an award ceremony based on nominees chosen by alumni and friends. The award categories include:
The Mary Elizabeth DeVasher Distinguished Alumni Service Award is awarded to a MTSA alumnus in honor of this MTSA alumnus and former Dean/Vice President/Program Administrator to celebrate and honor her years of dedicated work and distinguished service to the institution.
The Mission & Heritage Award is awarded to an individual who embodies and exemplifies the heritage, mission and core values of MTSA.
The Clinical Excellence Award is awarded to an anesthesia provider (anesthesiologist or CRNA) or clinical site (hospital, clinic, etc.) that provides a nurturing and exemplary atmosphere with true eagerness to instruct, train and educate MTSA students. The recipient will embrace the MTSA mission and core values.
The Nevin Downs Leadership Award is awarded to an anesthesia provider (anesthesiologist or CRNA) who personifies the integrity, honesty, fairness and exemplary leadership with which Dr. Downs served the profession including his advocacy of nurse anesthesia and MTSA.
White Coat Ceremony

Each year at its White Coat Ceremony, MTSA recognizes first-year students’ successful completion of the second semester of the DNAP program including skills testing and machine check off. Family and friends gathered at the Madison Campus Seventh-day Adventist Church as the Class of 2024 received their official MTSA lab coat.
MTSA Calendar
March 4 – 9th Annual Mission & Awards Gala
March 26 – Basic Regional Cadaveric Workshop [SOLD OUT]
May 1 – Deadline to apply to Doctorate Completion Program
May 1 – Deadline to apply to Acute Surgical Pain Management Fellowship
May 1 – Deadline to apply for Dual Enrollment (Doctorate Completion Program & Acute Surgical Pain Management Fellowship)
May 1 – Deadline to apply to Nurse Educator Certificate Program
May 7 – Advanced Regional Cadaveric Workshop
May 31 – Deadline to apply to Doctor of Nurse Anesthesia Practice Program
Sept. 10 – Basic Regional Cadaveric Workshop
Oct. 1 – Advanced Regional Cadaveric Workshop
For additional details, visit mtsa.edu/events.











