MTSA Fellow Publishes Case Studies from Army Deployment in Syria
November 1, 2019
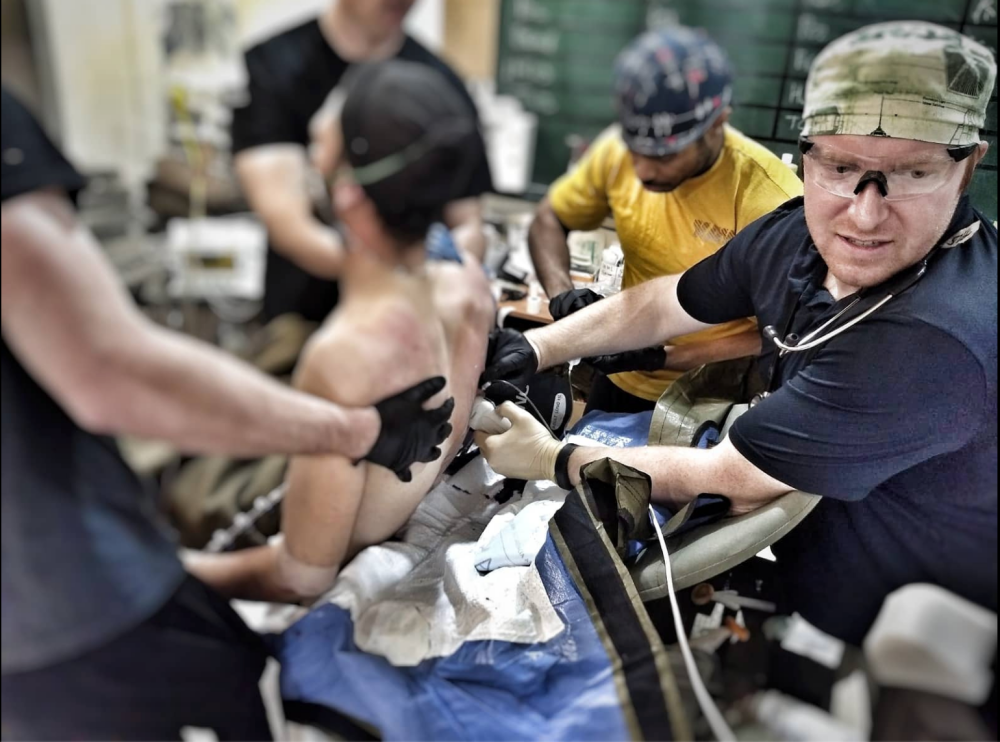
While deployed in Syria for 10 months during 2018-19, U.S. Army Major Robert Fabich, DNP, CRNA, saw more than 500 traumas and provided anesthesia care for 130 surgeries. During that time, he relied on his training from MTSA’s Acute Surgical Pain Management (ASPM) Fellowship to ensure his patients—both coalition troops as well as local nationals—received the best care possible in one of the most challenging settings imaginable.
Fabich leveraged his war-zone experience and developed two case studies, with the help of several colleagues, that have been recently published in Military Medicine:
- A Novel Use of the Erector Spinae Block in the Austere Environment (co-authors: Sharrod Greene, DNP, CRNA; Currie Tighe, BSN, RN; Rebekah Devasahayam, MD; and Tyson Becker, MD, FACS)
- Definitive Management of a Traumatic Airway: Case Report (co-authors: Benjamin T. Franklin, MD, and Nicholas Langan, MD)
“What’s unique about these cases is that the CRNA may be the only anesthesia provider in the room. There’s no backup,” Fabich said. “It’s a big responsibility because you’re doing a lot of major cases—open heart, vascular, abdominal—and all those emergency skills that you may have only talked or read about you may now have to do in a battle zone. So you have to be confident in your education and training.”
Fabich was part of an 11-member forward surgical team stationed in “Green Village,” supporting the troops on their final push against ISIS strongholds in Syria. Set up in an abandoned school house, the group started with only a couple stretchers and basic equipment. During their 10-month deployment, they converted the space into a makeshift hospital. The building didn’t always have electrical power and was not completely sealed off from the outside environment and weather.
“One of the issues we kept facing was that we needed to send our surgical patients with non-medically trained personnel for an ambulance ride to a local hospital for continuation of care. So we started brainstorming ideas for ways we could get them comfortable or in a position, which included being able to support their own airways, without a lot of narcotic so they would be safe along the way,” Fabich said.
Cases Published in Military Medicine
The case described in the Definitive Management of a Traumatic Airway involved the successful emergency management of a traumatized airway from a severe maxillofacial and neck-penetrating gunshot wound. The team consisted of two general surgeons, CRNA (Fabich), emergency room RN, two operating room technologists, two advanced trauma medics, and two intensive care LPNs. The case report focused on the importance of preparation, good communication, teamwork, and a strong knowledge base while working in the austere setting.
The focus of the Erector Spinae Block article was the case of a 25 year-old male with penetrating chest trauma. Due to limited resources and minimal monitoring in-transit, a regional anesthetic was placed for pain control. According to Fabich’s report, it is the first description of an erector spinae block utilized in a far forward combat setting.
Fabich said the experience helped him appreciate the utilization of newly acquired skills: “I learned how to do an erector spinae block during MTSA’s ASPM Fellowship. I thought to myself, ‘I think we can use this, which would enable us to not use narcotics.’ What it showed me is you need to be able to try new things safely and use what you’ve learned to the benefit of the patient.”
“Robert’s enrollment in the Fellowship was actually interrupted by his deployment to Syria,” said Bill Johnson, DNAP, CRNA, director of the ASPM Fellowship. “He used what he learned and put it to practical use in the field. He has been on the front lines providing life-saving care to injured troops as well as those less fortunate caught between battle lines. We’re glad he is able to come back and complete the Fellowship with this valuable experience under his belt.”
Hands-on Learning at MTSA
Commenting on the hands-on regional cadaveric workshops utilizing ultrasound, which is part of the Fellowship curriculum, Fabich said: “The labs were amazing. MTSA’s program goes beyond the basics, allowing us to think of other ways to approach cases, such as multimodal approaches to pain control and how to bring it into your practice. In terms of ultrasound, it’s probably one of the best cadaveric labs I’ve been to, especially with the pulsatile models.
“Through all these experiences, I’ve learned you always need to be ready to use that full skill set of anesthesia. You have to keep current and fresh. You can’t throw it on the back burner, because you never know when you’re going to use it again,” Fabich added.
Prior to joining the Army, Fabich received his BSN from Norwich University, attended the Army’s graduate program in anesthesia nursing, and earned his DNP from Northeastern University. A native of Bedford, N.H., he is married to Rebecca and currently serves as chief of the anesthesia department at Fort Wainwright in Fairbanks, Alaska.
Following are additional excerpts from our conversation with Robert Fabich:
What was a “typical day” during your deployment on the forward surgical team in Syria?
Robert Fabich: It would be difficult to describe a typical day because there was no such thing. But essentially you’d wake up in the morning—whether at 3 a.m. or 8 a.m., you never knew—to someone pounding on the door yelling, “Patient!” They’d come in and you go from 0 to 100 instantaneously, with these massive traumas. You bring them into the OR, then ship them out, then you clean up and hope you get 5 or 10 minutes to eat because there was no communication about when the next patient is coming. You’re always on edge, waiting. At the same time, there’s an active war going on, with missiles being fired right next to where we were trying to do surgery.
How did you manage in an environment where you didn’t have some of the basic supplies or equipment for the tasks at hand?
R.F.: From an anesthesia perspective, we would ask, “Can I get by with not using this medicine on this patient? I would normally administer it, but can I still do a safe anesthetic without it?” If the answer was “yes,” we might give half of the medicine we normally would give because I know I might need the other half for someone else. It’s definitely a situation where you have to improvise. You’re in the middle of a war zone. There’s no option for just ordering something on Amazon.
Any other cases that stand out in your memory?
R.F.: As our partner forces started gaining ground, we started to see more humanitarian cases – people who had been stuck in certain places and weren’t able to get out. So we started seeing more children and mothers. In one case, a woman came through the door, and we delivered her baby in that very moment. A lot of the kids started coming in and you just hopefully give a positive impact on a child’s life so maybe they remember that not everyone is bad in the world. That was always a good feeling when we could take care of them.
How did you choose to become a CRNA, and what does it mean to you to be practicing in the armed forces?
R.F.: I had a friend who was an ICU nurse and CRNA. He suggested I look into being a CRNA. So I shadowed him and thought it was really something I would like. It was a good mixture of critical thinking, making my decisions and doing a lot of procedures.
I feel like my role in the Army is a supporting role in a bigger picture. I take care of soldiers, providing the anesthetic so the surgeon can do surgery and that soldier can get back to doing their job, which in turn helps the country. On the back side of that, we also get to take care of our veterans and retirees, who have given so much for us.
For more information on MTSA’s Acute Surgical Pain Management Fellowship, visit www.mtsa.edu/fellowship.








